Do you suffer from acid reflux and take PPI’s?
Potential long-term impacts on your digestion and health
PPIs are a frequently prescribed medication for acid reflux. This blog looks into what they are prescribed for, how they work and possible side effects from long term use. Do you suffer from acid reflux and take PPI’s? If so, read on for information on the potential long-term impacts on your digestion and health.
What is Acid Reflux?
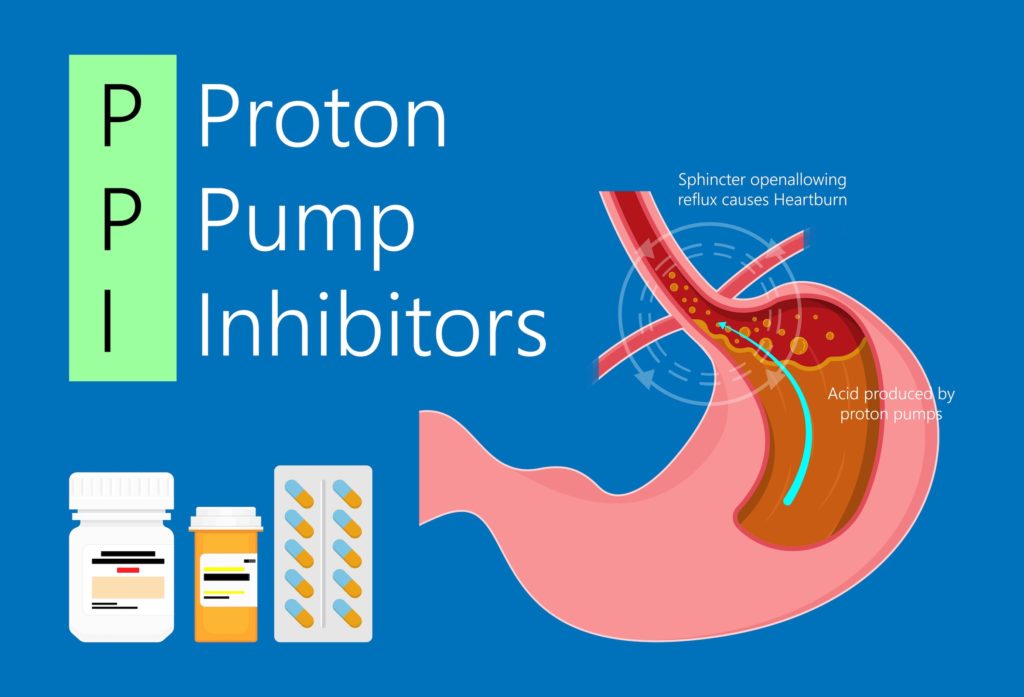
Our stomachs have a naturally acidic environment. Stomach acid is an essential part of the digestive process: protein breakdown begins here; absorption of B12 is started; iron, zinc, calcium, magnesium all rely on stomach acid for absorption. A thick, mucus-y layer protects your stomach from pain or erosion. If the acid stays in your stomach, then you generally don’t feel a thing (a gastric ulcer is another matter and not the focus of this blog).
When acid escapes
When acid escapes the stomach however, it is a different story. The oesophagus (the tube from mouth to stomach) literally burns when acid blows back up from the stomach, and in some circumstances, causes extreme discomfort.
Do you suffer from acid reflux and take PPI’s? Read on for more!
A thick, mucus-y layer protects your stomach from pain or erosion from the acid
When PPIs are prescribed
Enter PPIs. PPIs are a commonly prescribed medication for acid reflux. As many as 21% of the population has been prescribed a PPI over the past 30 years or so in the UK, mostly for heartburn. GPs have little else in their toolbox for heartburn and frequently prescribe Omeprazole or Lansoprazole (examples of PPIs) to offer some relief.
Acid Reflux and PPIs

For heartburn, PPI’s are often recommended daily for a period of 4 weeks. This can be extended for an additional 4 weeks if symptoms continue. After 8 weeks, further investigation is recommended. Often, nothing is found, and the PPI prescription continues. It is not uncommon for someone to be on these medications for decades.
With any medication prescribed to you by your GP, consultant or other healthcare provider, for whatever reason, you must discuss your drug regimen with them or your pharmacist before making any changes.
When PPIs are co-prescribed
It should be noted that PPIs are often co-prescribed with anti-inflammatory drugs (NSAIDs) to reduce the NSAID-induced gastrointestinal adverse effects. They can also be used if you have a gastric or duodenal ulcer.
It is essential that you discuss your overall drug regimen with your GP or pharmacist before making any changes
How PPIs work
Our stomachs contain proton pumps which pump out acid when our stomachs are getting ready to receive food. Messages are received by these pumps when we see food, touch it, smell it and anticipate eating. Our mouth waters for a reason – this process signals to the proton pumps that food is coming and to ramp up stomach acid production.
Do you suffer from acid reflux and take PPI’s?
PPIs ‘inhibit’ the action of these proton pumps. Hence, despite the signals being sent that food is coming, little acid is produced.
Common Side-Effects
Stomach acid plays a key role in our digestion. As well as protein digestion and absorption of key nutrients as mentioned above, others things are taking place in the presence of acid. The acidic mixture that passes from the stomach through to the top end of the small intestine stimulates the release of the next elements of digestion. Bile from the gallbladder is released and digestive enzymes from the pancreas. A highly acidic mixture leads to a strong production of these substances. Thus, absorption of all the lovely nutrients that you’ve eaten takes place, before being sent around the body to do their allotted tasks.
A weak acidic mixture does not stimulate the production of digestive enzymes to the same extent, compromising absorption
A weak acidic mixture does not stimulate the production of digestive enzymes to the same extent, compromising absorption. So, even if you are eating a nutrient dense, optimal diet, your absorption is compromised, with accompanying knock-on health impacts.

Long term Impacts
There are a significant number of side effects from PPIs use. Headaches, abdominal pain, constipation, diarrhoea, flatulence, nausea and vomiting are all listed as common undesirable effects. GPs are also advised to watch for magnesium deficiency with use of a PPI for more than 3 months and to monitor bone health for density when used for one year or more. These 2 impacts may well be linked, given the role of magnesium in bone health and density.
Overtime, B12 and iron deficiency may occur with accompanying fatigue, dizziness, hair loss, breathlessness and more. Suffice to say, long term use of PPIs for heartburn, unless required for other essential medications, is less than desirable.
Long term use of PPIs for heartburn, unless required for other essential medications, is less than desirable
Take Home Message
PPIs are most often prescribed because of the discomfort of heartburn after eating or whilst sleeping. The problem is not the stomach acid itself – we need that -, but the fact that the stomach acid is in the wrong place. PPIs reduce the production of stomach acid so there is less in the wrong place causing symptoms. Thus, it provides relief. However, the underlying cause of the acid being the wrong place in the first place is still there. Nothing fundamental has resolved.
There are ways to safely correct the underlying problem. Once this is achieved and under the care of your GP, you can then start to reduce your reliance on PPIs. You may start by reducing the dose and/or swapping to an alternative acid suppressant. This helps avoid rebound acid, which is common after using a PPI, even after as short a period as 3 days.
If you want to discuss this further, please you can book a free call with me. When a client is on prescription medications, I work exclusively in collaboration with your GP, to support your digestion and mucus secretions whilst reducing, and finally stopping, your PPI.
If you want to read other blogs I’ve written on stomach acid, check out this one Heartburn, Medications and the role of your stomach acid.
Sometimes, reducing your carbohydrate intake can help with reducing acid reflux. Check out this eBook with 10 delicious recipes focusing on cruciferous vegetables, including substitutes for rice and mash potatoes.
